Address: VGM Hospital, 2100/2, Trichy Road,
VGM Hospital Bus stop, Singanallur,
Coimbatore, Tamil Nadu 641005
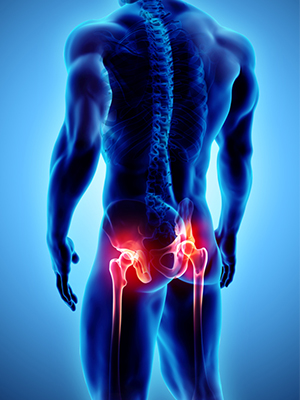
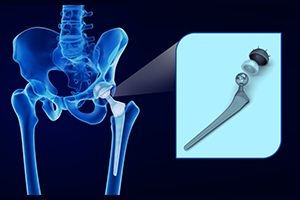
The Hip Joint is a ball and socket joint made up of the spherical structure (head of Femur) and the socket (called Acetabulum). The bones are lined by a smooth layer called articular cartilage to allow smooth,pain free and low-friction movement of the bearing surfaces.
The Hip Joint has both stability and mobility. From inside to outside, the hip joint is enveloped by layers of tissues called synovium, capsule, ligaments, muscles, fat and skin. The synovium produces synovial fluid for lubrication. The capsule and ligaments are the primary hip stabilisers giving stability and allowing limited range of movement. They prevent the joint from getting dislocated. The muscles are secondary stabilisers and also aid in movement.